COVID-19 Monitoring Project (2020) — Legacy page
Archived daily graphs and short notes (March–June 2020) for selected countries covering case counts, testing volume, doubling times, fatalities, CFR vs IFR, hospital capacity, and simple scenario modelling. Maintained as a sample of our consulting/analytical writing and modelling work.
Legacy page (archived). This page documents our 2020 COVID-19 monitoring project and is no longer updated. Content reflects information and policies as of 5 June 2020. Some figures continued to update automatically with data from the ECDC and other sources until about June 2022 (figures only—not the text). This page is retained solely as a sample of our data analysis and modelling capabilities. For current services, see our Science Consulting and Modelling Projects pages.
A message from the XpertScientific team
As we have been receiving enquiries as to our operational capabilities during the current crisis we have set up this page to provide some information about whether and how XpertScientific and our services are affected.
We do not currently expect any disruption to our service and should be able to continue operating at normal capacity.
- All our client communication is online and will not be affected
- Remote working has always been part of our company culture, and this will not impact our operational capacity
While we don't expect any issue in the foreseeable future, we will of course notify you before accepting payment for a specific order if there are any changes to our usual service or turnaround times.
We wish you the necessary strength and good health to master this crisis.
Your XpertScientific Team
Monitoring case numbers and fatalities in selected countries
Contents
As a science consultancy, we want to keep an eye on the progression of this outbreak and decided to share some graphs and analyses for a small selection of countries to monitor the evolution of total case numbers, doubling times, testing capacities, fatalities, recovered cases, and indicative levels of herd immunity. This is not intended as a rigorous scientific analysis but a leisurely look at the numbers by two data scientists.
Comparisons between countries are tricky as each country applies different rules to testing and reporting so please bear this in mind when viewing the following graphs.
All text and plots are © XpertScientific. Please get in touch if you wish to use a particular figure in your publication.
Vaccinating against SARS-CoV-2
Testing for SARS-CoV-2
The number of tests is arguably the most important parameter as only high-volume testing will provide a sufficiently accurate picture of case and fatality numbers. In fact, officials from several countries have already admitted that due to insufficient testing the officially reported case numbers may grossly underestimate the actual numbers (by factors ranging from 10 to 20 depending on the country). This is also supported by the high percentage of positive tests in many countries and the high case fatality rates (see below).
Not all countries publish regular updates on their testing and it is often unclear what the numbers actually represent. Some countries report people while others report the number of PCR tests or swabs. There may also be repeat tests for some individuals (such as hospital and care workers).
- The UK publishes the number of different people tested, i.e., individuals.
- Sweden and South Korea report the number of people tested although without specifying whether the numbers contain repeat tests of the same individuals. Sweden publishes test numbers only once per week.
- Germany and France report the number of tests which is ambiguous and could refer to either specimens or people. They both only publish their numbers once per week. Since January 2020, Germany has also added routine testing for SARS-CoV-2 to its ongoing antibiotic resistance surveillance where participating labs, while carrying out their regular blood work, also tested for a range of potentially dangerous pathogens. From about half a million tests (as of 14 April 2020) 8.6% were positive for SARS-CoV-2.
- Italy reports the number of tamponi (literally "swabs"). Considering that they recently added a new category labelled "casi testati" (tested cases - about 30% lower than the number of swabs) it seems likely that swabs refer to specimens. As there is only a complete time series for swabs we decided to plot those in the figure below.
- Data from the US are difficult to interpret and have inconsistent units as they originate from a wide mix of private and public labs and clinics and different states report the data in different ways (some as specimens, others as people tested, some including pending and negative tests, others not, etc.). We therefore did not even attempt to estimate the actual number of people tested but are simply showing the reported numbers (bearing in mind that they represent a mix of specimens and people).
- Spain until recently did not publish any official numbers on testing. Now they provide weekly numbers on tests, i.e., most likely specimens rather than people.
Comparing Doubling Times
The doubling time of confirmed cases gives an indication of how quickly an outbreak is spreading. At the beginning of the SARS-CoV-2 outbreak cases would double every 2-3 days (or even daily in South Korea - see below). As a result of the applied mitigation measures such as social distancing (which is really physical distancing), contact tracing, and the closure of large parts of the economy as well as all cultural and educational institutions, countries tried to slow the spread of the virus and thus increase the doubling times, with considerable success as can be seen below.
Comparing Fatalities and Case Fatality Rates
The case fatality rate (CFR) can be calculated as:
CFR =number of deaths from a disease/number of diagnosed individuals with the disease × 100 (in %).Having been tested positive for the SARS-CoV-2 virus does not mean that you will necessarily develop the COVID-19 disease. While the CFR is frequently cited in the media, it does not actually provide any information about the mortality or the risk of dying if you have the virus. The former, often called crude mortality, is the number of deaths from a disease divided by the total population, while the latter is usually referred to as the infection fatality rate (IFR):
IFR =number of deaths from a disease/number of infected people × 100 (in %), i.e., the denominator contains all infected people including the asymptomatic cases that do not develop the disease, a figure that is inherently difficult to know. The relatively high CFRs in some countries suggest that the disease went undetected there for some time and the dark figure may still be considerable as the actual IFR is expected to be around 0.37 to 0.5%.
Hospital Beds
Before looking at the individual country data, it may also help to briefly examine the capacities of each country's health system, represented here by the number of hospital and ICU beds. Given that a sizeable percentage of patients requires hospital or even ICU care, the number of beds provides some indication of how quickly an overflow/triage situation could arrive. While Germany and South Korea seem to have mastered the first wave of infections without even approaching the limits of their health systems, the rather low bed capacities in the UK, Italy, and Spain meant that under "normal" conditions they would already be operating at high occupancy percentages and an outbreak such as COVID-19 quickly brought hospitals to their limits which may partly explain the high number of fatalities in those countries. In eastern France, news reports stated that at some point patients over 80 years of age were no longer put on life support as hospitals were running out of respirators. Sweden also has a relatively low per-capita number of hospital and ICU beds; however, the country did not appear to have exceeded its capacity at the time of writing.
Country Data
Spain
We start with Spain as we are located in Barcelona. Spain imposed some of the strictest measures, not only closing schools, shops, and cultural venues (starting from 15 March 2020) and even all its non-essential factories (for 2 weeks from 30 March till 12 April 2020), but in contrast to its central and northern European neighbours, people in Spain were also forbidden to go outside for walks or daily exercise. City and forest parks as well as beaches were off limits confining the public to their homes or the streets while purchasing the bare necessities. It is also the only European country that completely banned all children from going outside for over 6 weeks. Nevertheless, Spain has one of the highest per-capita numbers of deaths and cases in the world.
Note: If you follow the official Spanish numbers, you will have noticed a reduction in case numbers by about 11,000 on 24 April 2020. This is because Spain stopped including positives identified using antibody tests in its official totals and, as of 26 April 2020, no longer publishes the total number of antibody positives (only graphs).
Germany
Compared to its European neighbours, Germany seems to have coped fairly well with this outbreak and could take on over 200 ICU patients from neighbouring France and from Italy where hospitals had exceeded their capacity. By learning from the South Korean experience and approach, Germany ramped up testing early and carried out rigorous contact tracing and quarantining. Unlike people in Spain, Germans were never confined to their homes and could keep using city and forest parks as well as beaches for daily walks and exercise which seems a sensible measure as it allowed people to maintain a basic level of fitness which also benefits the immune system. On 17 April 2020, the government announced that the outbreak was "under control" as the basic reproduction number, R0, had dropped to about 0.7 (meaning that every infected person was infecting less than 1 other person, a necessary condition to contain an outbreak). As a result, most small shops were allowed to reopen on 20 April 2020.
While the per-capita case numbers are comparable to other European nations, their CFR is much lower (see above) suggesting that their dark figure may be lower as well. This lower CFR may be partly due to the early high-volume testing (the more cases that are identified the more the CFR approaches the IFR) and partly to the fact that many of the initial positives were relatively young.
Italy
Italy was one of the first European countries to register a case of COVID-19 in a Chinese couple that had arrived from Wuhan at the end of January 2020. Five weeks later, on 8 March 2020, 15 provinces were placed under lockdown, a measure that was extended to the entire country only 2 days later as people from affected areas had begun to travel en masse to the provinces not yet under lockdown. On 21 March 2020, Italy halted all non-essential production, industries, and businesses. The lockdown has been slightly relaxed in early May 2020 and the country has reopened to tourism in early June 2020.
There are some inconsistencies in Italy's official numbers on fatalities and the country is currently reviewing them. We provide some speculation on the actual numbers below.
France
France was the first European country to have a confirmed case of COVID-19 in a recent arrival from China (on 24 January 2020). France began a national lockdown on 16 March 2020. As of 23 March 2020, all people were required to carry a piece of paper that contained the reason for having left home and fines were imposed for non-essential journeys although people were still allowed to go out for exercise (1h per day within 1km of their residence).
In response to news reports criticising France for only reporting cases and deaths from hospitalized patients, France has moved to include cases and deaths from care facilities from 3 April 2020 which is not reflected in the data series below (from Johns Hopkins University) until 12 April 2020 when a significant increase occurs. Some portals like the ECDC continue to report the lower hospital-only number. In early June 2020, France started to relax the lockdown measures.
United Kingdom
The UK reported its first 2 cases on 31 January 2020 among a family of Chinese nationals staying in the country. Overall, the country was slow to impose mitigation measures and the stated government policy initially intended to achieve herd immunity as quickly as possible, apparently unaware of the rather catastrophic death toll this would entail. By mid March 2020, when countries on the continent were about to go into lockdown, the UK was still holding a 4-day horse racing event with about 250,000 attendees. As case and fatality numbers continued to rise, cultural venues and restaurants were eventually closed on 20 March 2020 and three days later a full lockdown was imposed.
Until 29 April 2020, the UK only reported deaths from hospitals. As of 30 April 2020, official data also started to include deaths that occurred in care facilities and private homes and the entire data series has been updated accordingly. The reason for the high UK CFR is most likely due to the fact that the country initially performed very few tests.
United States
The US recorded its first case on 20 January 2020, i.e., before any European country, in a citizen that had returned from Wuhan, China. The government response was rather slow. Despite having imposed a travel ban on China as early as 31 January 2020, US president Donald Trump continued to downplay the seriousness of the threat and for a long time claimed that the situation was "under control" and the number of infections would be "close to zero" within "a couple of days". However, scientific reality does tend to catch up with even the most hardened of demagogues and science deniers; in an about-face on 11 March 2020, Trump was forced to announce that the situation was "not under control".
The mitigation response varied from state to state ranging from lockdowns with school, shop, and industry closures to no mitigation whatsoever. After a slow start, the testing capacity was ramped up quickly and significantly with about 150,000 daily tests being performed at the time of writing. By 22 April 2020, Trump started to advocate an end to the statewide lockdowns and many measures have been relaxed although the number of new cases (and doubling times) did not justify any relaxation of the mitigation measures.
South Korea
South Korea confirmed its first case on the same day as the US, i.e., on 20 January 2020, and also in a Chinese national from Wuhan. After increasing slowly at first, in late February 2020 the numbers jumped by a few hundred as a result of a large religious gathering which eventually proved responsible for about 50% of all cases nationwide at the time. In response, the government quickly isolated and contained the cluster. In fact, most of the success in South Korea has been attributed to their high volume testing as well as rigorous quarantining of localised clusters and their immediate contacts. As a result, South Korea has by far the lowest per capita numbers in this comparison, even without having to impose any significant restrictions on the mobility of the general population, the country's economy, or cultural institutions which all remained open. Despite new infections having dropped to near zero, the country continues to test about 5000-8000 people per day.
Sweden
Sweden confirmed its first official case on 31 January 2020 in a woman who had arrived from Wuhan, China. This first case was successfully contained and no new cases were reported for almost one month until a second case was reported on 26 February 2020 in an arrival from northern Italy. Since then cases have risen more rapidly. Sweden is an interesting case as it is the European country with the least severe mitigation measures. Apart from the usual recommendations about handwashing and social distancing—which is really physical distancing—both social and work lives in Sweden continued almost unaffected except that gatherings of more than 50 people were forbidden, leading to the closure of high schools and universities. However, museums, primary schools, pubs, restaurants, malls, shops, and even gyms have remained open. The government has justified this approach with the "self-restraint" and "sense of responsibility" of the Swedish people, stating that "our whole system for communicable disease control is based on voluntary action". While it is admirable that Sweden places this much trust in its citizens, the country has had more deaths per capita than any of its Scandinavian neighbours and doubling times that are shorter than anywhere else in Europe.
If we were to speculate ...
As we all eagerly await a return to normality, we tried to assemble different pieces of the puzzle to be able to venture an educated guess regarding the current situation and the level of immunity reached.
What we know at the time of writing (5 June 2020):
- Dark figure: there is a dark figure in both the number of cases and the number of deaths. As the name implies, this figure is inherently difficult to pin down. One of the approaches to obtain an estimate for the true number of cases is through large-scale antibody testing of representative samples of the population. To determine the dark figure in the number of deaths, national health authorities often resort to the so-called excess deaths. This term refers to the number of deaths that exceed (statistically significantly) the multi-year baseline, e.g., say the normal March mortality is 100 (+/-20 of inter-annual variability) and in one particular year the figure suddenly becomes 250 then there is a statistically significant difference in the number of deaths. Excess deaths are routinely used to gauge the full size of influenza and other epidemics.
Table 1 - Using data collected by the NY Times on excess deaths, the number of official COVID-19 related deaths, and the resulting correction factors. Country Period (2020) Excess deaths Official COVID-19
related deathsCorrection
factorSpain 16 Mar - 10 May 43,700 26,570 1.64 Germany 16 Mar - 26 May 3,000 5,737 n/a Italy March 24,600 13,710 1.80 France 16 Mar - 26 Apr 24,300 22,708 1.07 UK 14 Mar - 15 May 59,200 45,226 1.31 US 15 Mar - 26 Apr 63,700 47,430 1.34 Sweden 16 Mar - 10 May 4,300 3,594 1.11 - Infection fatality rate: A study on the Diamond Princess cruise ship suggested an IFR of 0.5%, while a case cluster study in a heavily affected German town suggested an IFR of 0.37%. A large-scale antibody study in Spain found that 5.2% of the population had antibodies, i.e., contracted COVID-19 (as of 5 June 2020). Together with the "true" number of deaths that can be estimated from the excess deaths (s. above) this would yield an IFR of 1.83%, i.e, a value near the upper end of the spectrum of the available estimates. As this is the largest and most comprehensive study available to date, we chose to use this IFR value to gauge the level of immunity reached in our selection of countries. We are of course aware that the above scaling factors are educated guesses at best and wild speculation at worst and that the IFR may differ depending on the geographical and cultural settings. We therefore applied some sizeable error bars to account for the variability in IFR (using the German value of 0.37% as lower bound - corresponding to the upper end of the error bars) and scaling factors. We can derive some reassurance from the fact that our guesses yielded immunity levels for Spain and Italy that are in the same ballpark as projections by a widely used epidemiological model (see below).
Estimating the percentage of the population that is currently immune against SARS-CoV-2 from an estimate of the "true" deaths and an IFR of 1.83% (see text). Symbols are estimates for 18 April 2020 from the study by Delius et al. (2020). Note: for SARS-CoV-2, herd immunity is reached once about 66% of the population are immune. Epidemiological Modelling
Apart from educated guesses and wild speculations (see previous section) we can of course also employ some of the available epidemiological models. However, the authors of these models often need to resort to the same guesses and estimates when trying to constrain their model parameters. Nevertheless, these models provide a valuable tool to run through different scenarios which may aid decision makers to devise mitigation measures and exit strategies from the current lockdowns. We found the model from Neher et al. rather easy to use as they provide a simple web interface where visitors can tune some of the model parameters to generate different scenarios. At the time of writing, the web interface did not allow users to specify any correction or scaling factors to account for the dark figure in case and death numbers which would be useful for fitting the model to "corrected" official data.
We tuned the model parameters to obtain the best possible fit to the "true" number of deaths using the correction factors from Table 1 above. We also added mitigation measures to mimic those imposed by the local governments such as general lockdowns and industry closures. We also tried to account for a delayed increase in awareness in the population.
Simulation results using the epidemiological model by Neher et al. (Univ. Basel) comparing the effect of (a) mitigation vs (b) no mitigation for the Spain scenario. Model parameters were tuned for a best fit to the number of official deaths + 60% (see text and Table 1). The discrepancy in total cases, especially in Feb/Mar, could be due to Spain's delayed response and lack of testing. In (a) we simulate the three types of mitigation measures that were imposed in Spain: (i) general lockdown starting on 15 March 2020 with closure of all schools, shops, and cultural venues. People are only allowed to go outside to commute to and from work and to buy essential items like food. Children are not allowed outside for any reason. As people were a little slow to adopt this lockdown, we used a reduced effectiveness of 55% for the first week, increasing to 75% by the second week. The effectiveness indicates the percentage by which Ro is reduced. (ii) On 28 March 2020, Spain also closed all its factories and non-essential businesses for 2 weeks. We added this as a second mitigation measure with an (additional) effectiveness of 60%. (iii) The strict lockdown started to be relaxed from about 8 May 2020 but some restrictions remain in place, plus the heightened awareness in the population, the wearing of face masks, and other measures to improve hygiene in supermarkets and shops will maintain a level of mitigation of 67%. (b) Without mitigation the epidemic could be over by mid-June 2020 but there would be over 650,000 deaths. The chosen mitigation measures thus saved over 600,000 lives. To check whether the good match between the model and our simple scaling method for the Spain data was perhaps a fluke, we also fitted the model for the Italy scenario to the number of deaths scaled by 1.8 (see Table 1). Again, the level of immunity predicted by the model and our scaling method are in fairly good agreement.
Simulation results using the epidemiological model by Neher et al. (Univ. Basel) comparing the effect of (a) mitigation vs (b) no mitigation for the Italy scenario. Model parameters were tuned for a best fit to the number of official deaths + 80% (see text and Table 1). In (a) we simulate the three types of mitigation measures that were imposed in Italy: (i) general lockdown starting on 9 March 2020 with closure of all schools, shops, and cultural venues. As people were slow to adopt this lockdown, we used a reduced effectiveness of 50% for the first week, increasing to 70% by the second week (original Ro=4.2). (ii) On 22 March 2020 Italy closed all its factories and non-essential businesses until 3 May 2020. This has been added as a second mitigation measure with an (additional) effectiveness of 62%. (iii) Once industry closures ended on 3 May 2020, some restrictions remained in place, plus the heightened awareness in the population, the wearing of face masks, and other measures to improve hygiene in supermarkets and shops will maintain a high mitigation effectiveness of 70% throughout summer. (b) Without mitigation the epidemic could have been over by mid-June 2020 but there would be about 950,000 deaths. With the chosen mitigation measures about 900,000 lives could be saved. Finally, and to test whether our decision to not use any scaling was justified for Germany, we also fitted the model to the Germany scenario using the number of official deaths (unscaled - see Table 1). The level of immunity predicted by the model and our scaling method are again in the same ballpark.
Simulation results using the epidemiological model by Neher et al. (Univ. Basel) comparing the effect of (a) mitigation vs (b) no mitigation for the Germany scenario. Model parameters were tuned for a best fit to the number of official deaths (unscaled - see text). In (a) we used two mitigation measures, (i) a partial lockdown closing nurseries, schools and universities, and cancelling mass events reducing the initial Ro by 40%, and (ii) a second suite of measures forbidding gatherings of more than two people and closing cultural venues, restaurants, shops and services, reducing Ro by an additional 65% (to achieve an Ro=0.7 as estimated by the Robert Koch Institute for 18 April 2020). Without mitigation the epidemic would be over by mid-June 2020 but there would be over 1.2 million deaths. With the chosen mitigation measures the number of deaths is just a fraction (~9,000), i.e., about 1.2 million lives were saved. When comparing the Spain, Italy, and Germany scenarios it becomes clear how important the timely introduction and duration of mitigation measures are for reducing the number of fatalities. While Germany introduced its first set of measures when the official deaths stood at just 17, Italy and Spain only did so when official deaths were already in the hundreds. This kept hospitalizations in Germany low (the number of severely ill cases there never exceeded ICU capacity).
We reran the model for Spain introducing all measures one week earlier (not shown), which resulted in a reduction in the number of deaths by about 75%.
One possible reason why Italy has fewer deaths than Spain (despite having about 30% more inhabitants) may be the duration of the industry closures: 2 weeks in Spain versus 6 weeks in Italy.Effect of the COVID-19 crisis on emissions
One interesting aspect of the coronavirus crisis is the reduction of CO2 emissions and pollution as a result of the economic slow-down and travel restrictions. The figure below shows how pollution ((nitrogen dioxide, NO₂) levels have cleared in the lower atmosphere over China due to a decline in traffic and industrial production. While this only provides a temporary relief, its impact on the planet and the different ecosystems may be sufficiently large to warrant more detailed studies and future publications.
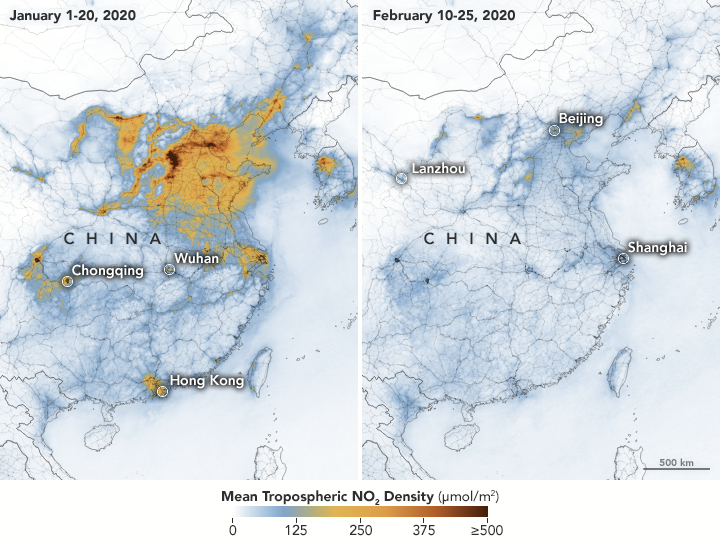
Reduction of nitrogen dioxide (NO₂) in the lower atmosphere over China as a result of the COVID-19 crisis. Source. 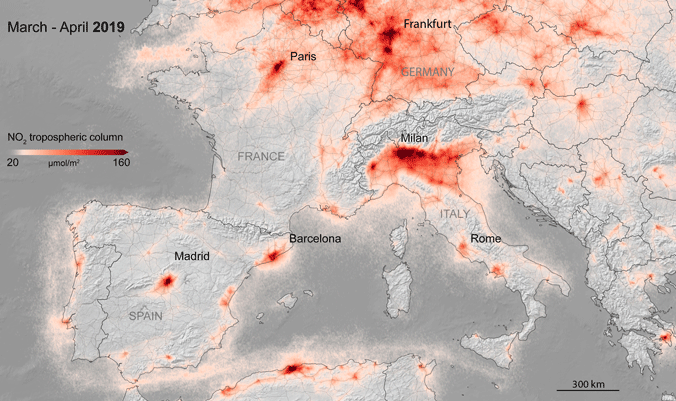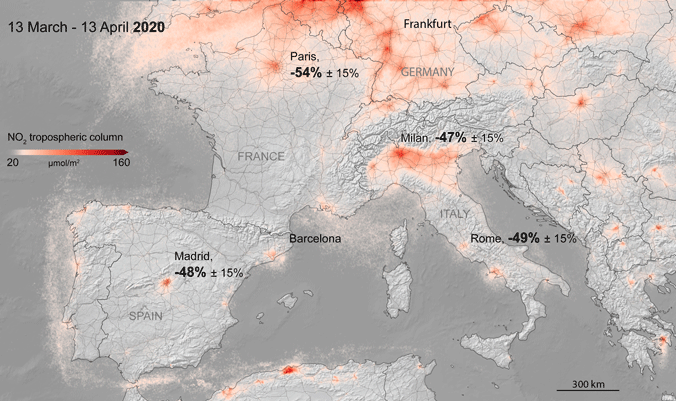
Reduction of nitrogen dioxide (NO₂) in the lower atmosphere over southern and central Europe as a result of the COVID-19 crisis. Source. Data Sources
- Cases, deaths, and recovered from Johns Hopkins University Center for Systems Science and Engineering data repository at https://github.com/CSSEGISandData/COVID-19
- Test data from Our World in Data repository at https://github.com/owid/covid-19-data/tree/master/public/data/testing
- Epidemiological modelling using the Neher et al. model v 1.2.0 https://covid19-scenarios.org/
For other individual sources see the main text.